How Do Nicu Preemie Babies Regulate Their Body Temp
Introduction
Torso temperature command is of outmost importance in preterm neonates. Both hypo- and hyperthermia are known to negatively touch on their brusque- and long-term outcome. Therefore, considerable efforts are made in neonatal care to go along the babies' body temperature in the "normal" range. However, scientific evidence on what might exist the "normal" body temperature in preterm neonates is largely lacking.
In utero, the fetal temperature is higher than the maternal temperature (1–iii). For term babies the World Health Organization (WHO) recommends a body temperature range of 36.5–37.5°C (4). Some authors propose to apply the same reference range to preterm infants, likewise (5, 6). However, most clinical studies on preterm infants' oestrus residuum take been published decades ago when limitations in neonatology were much greater than they are today (7–10). Moreover, the bulk of papers on neonatal thermoregulation deal with body temperature on admission or during the beginning hours of life and its influence on short-term outcome parameters such every bit mortality (5, vi, eleven, 12). Very little, if any, is known nigh the optimal target body temperature of preterm infants during their stay on the Neonatal Intensive Intendance Unit of measurement (NICU), and its potential influence on long-term consequence parameters such as neurological evolution. Practical recommendations on how to arrange the ambient conditions for preterm neonates, in social club to provide "thermoneutral care," are given in relevant textbooks (thirteen–fifteen). Notwithstanding, in a French survey published in 2012 including a full of 186 NICUs information technology was shown that the variability of thermal management in daily routine was yet large and often not adjusted to the infants' historic period and maturity. Main incubator settings for temperature and relative humidity were distributed very heterogeneously (xvi).
In view of these findings, we conducted a survey to assess routine practices of thermal care and, to a higher place all, torso temperature targets in very low birth weight infants (VLBWI) among high-level NICUs in Deutschland, Switzerland, and Austria.
Materials and Methods
The survey instrument was a specifically designed online questionnaire. The software tool Survey Monkey® was used for survey design, distribution, and recollection of data.
The questionnaire consisted of 21 questions covering the following items: demographics, temperature target range, temperature measurement methods, estrus therapy devices including style of functioning, standards and complementary methods of thermal care. Within the demographics section, the size of the NICU and the number of infants < ane,500 g admitted per yr were recorded as well as the staff position of both the answering participant and the flagman primarily responsible for thermal management on the specific NICU. With regard to the temperature target range, body core temperature and definitions of hypo- and hyperthermia were addressed. Here, temperature range and cut-off points for hypo- and hyperthermia were provided in predefined temperature intervals of 0.5°C. For farther specification in the temperature target range and heat therapy devices sections of the survey, the neonates were categorized into iii exemplary subgroups according to their gestational age (GA) and nascency weight (BW): (one) 30 weeks of gestation (WOG)/1,500 thousand, (2) 27 WOG/1,000 thousand, (three) 24 WOG/500 m (Figure one; cf. also Information Sheets ane and ii in the Supplementary Material).

Effigy 1. Sample question from the online questionnaire on thermal management in three different categories of VLBWI (Question #6: Target body temperature): Participants were asked to check all boxes/temperatures that would be deemed acceptable on their NICU.
A pretest of the survey in order to evaluate its comprehensibility and feasibility was run among the medical and nursing staff of the Sectionalization of Neonatology and Pediatric Critical Care Medicine in our institution. The finalized survey version was sent out betwixt Oct 2014 and Jan 2015 and was addressed to the respective head neonatologists of 149 perinatal 3rd care centers, including 136 German language, half dozen Austrian, and 7 Swiss centers. It was her/his decision to answer the survey past herself/himself or to requite it to one of the section'southward staff physicians, caput nurses or certified nurses. Only one member of each middle was immune to answer the survey, regardless of its professional group (head neonatologist, staff dr., caput nurse, certified nurse). Selection of participants was conducted via an internet-based systematic enquiry. In Germany, perinatal "level one" centers are divers as centers which regularly care for infants <1,250 g and which provide a minimum of vi NICU beds including respiratory back up options. Only perinatal centers "level one" were included as participants in Deutschland. To ensure comparability all Austrian and Swiss centers were selected by applying the same criteria. A maximum of two electronic reminders were sent every xv days to all centers with a awaiting reply. But one answered survey per participating centre was eligible for analysis. Eligibility for analysis was given if more than the first five questions of the survey were answered.
Statistical Analysis
We used chi-squared tests to compare qualitative variables and an analysis of variance to examination quantitative variables with the use of a post-hoc Fisher'southward protected to the lowest degree square difference exam if F-values were pregnant. Pearson coefficients (r) were calculated for the correlation between selected variables. The statistical significance threshold was prepare to p < 0.05. Information are presented equally counts and percentages or as hateful ± SD, and inter-level variability is expressed as the coefficient of variation (CV) which is SD divided past the mean. All analyses were performed using SPSS 22 (IBM Corp., Armonk, NY, USA).
Results
The survey return rate was 75% (n = 112). A total of 25 answered questionnaires (22%) had to exist excluded from analysis. Reasons for exclusion were: multiple answers from the same participating center (n = 21) and incomplete response (less than first five survey questions answered) (n = 3). Since only 2 out of six Austrian NICUs returned an answered questionnaire of which 1 contained an incomplete response, the analysis was confined to German and Swiss centers. Finally, 87 returned questionnaires were included into statistical assay (58%). Of those, 82 (94%) contained a complete and five (6%) an incomplete response.
The mean size of the participating NICUs amounted to 16.2 ± half dozen.six (median fifteen) beds, the hateful number of treated VLBWI to 59.2 ± 41.8 (median 50) neonates per twelvemonth. The survey was mostly answered by the head neonatologist (n = 64; 74%) or the caput nurse (n = 11; 13%) of the respective department whereas in the majority of centers, the temperature direction was performed by the nursing staff at bedside (n = 76; 87%) (Table ane). Well-nigh one-half of the centers (northward = 34; 41%) based their thermal direction decisions on clinical bedside assessment, almost others (north = 37; 45%) written report the use of standard operating procedures (SOPs).

Table i. Demographics of the online survey: The questionnaire was mainly filled by head physicians or head nurses whereas thermal management is mostly performed by (certified) nurses at bedside.
In the majority of centers (northward = 60; 69%) temperature measurement was conducted continuously, more often than not by using a skin probe either attached to the dorsum/lying surface (43%) or to the anterior belly of the infant (28%). Rectal probes were less oft used for continuous temperature monitoring (8%). Gradient measurement, measuring the gradient between the primal and peripheral torso temperature with a sensor placed on the anterior abdomen and another on the sole of human foot, was but used by sixteen% of the centers. Xxx-ane percent of the centers reported the utilise of intermittent rectal temperature measurement using a digital thermometer.
The reported target torso temperature range was like across all GA and BW categories and amounted to 37.02 ± 0.2°C (24 WOG/500 g), 36.99 ± 0.22°C (27 WOG/1,000 yard), and 36.98 ± 0.17°C (thirty WOG/1,500 m), respectively (mean ± SD), with a common boilerplate of 36,99 ± 0,19°C (Figure 2). Inter-middle variability was depression with a variation coefficient of one%. Overall, if answering, the head nursing staff designate a higher target range for body temperature in preterm infants compared to the answering head physicians (p = 0.003) or answering staff physicians (p = 0.015).

Figure 2. Target trunk temperatures for preterm neonates on loftier-level NICUs: Number of positive answers and normal distribution in three different categories of VLBWI. As in term babies, 37.0°C is presumed to be the normal body (core) temperature for VLBWI, nearly irrespective of gestational age (in Weeks Of Gestation, WOG) and/or birth weight (in grams).
Hypothermia was divers homogenously across all three preterm babe categories, with a non-significant trend toward a higher temperature cutting-off bespeak in the smallest category of preterm infants (24 WOG, 500 m) compared to infants of xxx WOG, i,500 g (Figure iii). Again, inter-center variability was depression with a variation coefficient of 1%. Answering head nurses (p = 0.001) and certified nurses (p = 0.04) ascertain a higher temperature value every bit hypothermia than the answering caput physicians (means: 36.65 and 36.threescore°C, respectively, vs. 36.46°C). If thermoregulatory determination-making is based on clinical bedside assessment only, hypothermia was defined earlier, i.e., at higher temperature values than when based on recommendations from the scientific literature (p = 0.007).
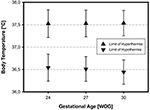
Figure 3. Definition of hypothermia and hyperthermia in three unlike categories of VLBWI. The corresponding temperature limits (means ± SD) reflect the assumption that 37.0°C is normal, contained of gestational historic period and/or nascency weight (in Weeks Of Gestation, WOG)—except for a slightly higher limit of hypothermia in the nigh immature neonates.
Hyperthermia was divers similarly beyond all centers (variation coefficient 1%), and was equally independent of the infant's GA and torso BW (Figure 3; cf. also Table S1 in the Supplementary Material). If the thermoregulatory decision-making was based on clinical bedside assessment only, hyperthermia was considered earlier, i.east., at lower temperature values, compared to the use of SOPs (p = 0.002).
All participating centers used the incubator rather than the rut radiator equally heat therapy device. Sixty-viii percent (n = 59) prefer the air temperature control mode (ATC) to the skin servo-control mode (SSC) (north = 27; 31%) in routine exercise.
In the ATC manner of incubator care, the air temperature on admission depended on the infant's GA and BW. The smaller and more than immature the infants, the college the selected air temperature levels. The inter-center variability was three%. The relative humidity on admission also depended on the infant's GA and BW, with higher humidity levels being chosen in smaller and more young infants. These differences were highly significant (p ≤ 0,001) (Figure 4). There was a significant positive correlation (r = 0.385, p = 0.004) between ambient temperature and relative humidity in the almost immature babies (24 WOG/500 g) indicating that those, who prefer higher ambient temperatures, also aim at higher relative humidities. The inter-centre variability for incubator humidity levels was high with a variation coefficient of 11%, highest for infants of 30 WOG/1,500 one thousand with a variation coefficient of 12%. Smaller centers (≤l VLBWI per year) chose significantly lower humidity levels than centers with higher patient volume (p = 0.004).
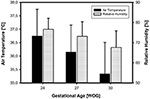
Figure 4. Incubator settings (on admission to the NICU) in three dissimilar categories of VLBWI. There is a articulate increase in both air temperature and relative humidity (ways ± SD) with decreasing gestational age (in Weeks Of Gestation, WOG) and/or birth weight, in accordance with common textbook recommendations.
In the SSC mode of incubator care, the air temperature on admission was similar beyond all preterm infant categories (p = 0.97), smaller centers chose significantly higher temperature levels than centers with higher patient volume (p = 0.004). The relative humidity values on admission depended on the baby'due south GA and BW (p < 0.001). Again, a relevant inter-eye variability could exist seen, especially in infants of thirty WOG/1,500 g (variation coefficient 10%) (p ≤ 0.001).
Discussion
Evidence-based guidelines on the appropriate body core temperature for preterm neonates are largely defective. It was therefore to exist expected that the thermal direction practices would show some heterogeneity across the different institutions. Surprisingly, all the same, the target body temperature data nerveless in this survey showed a very uniform normal range of 36.6–37.iv°C (hateful ± ii SD). Too, the definition for hypo- and hyperthermia was very like for all preterm infants, contained of GA and BW.
The unanimously preferred temperature corresponds to the normal range of body temperatures the WHO defines for term infants (4). Recent studies advise that this temperature target range could be appropriate for preterm infants, too: In 10 small preterm infants Knobel et al. (5) observed that a body temperature range of 36.viii–37.0°C maximized normal middle charge per unit recordings during the first 12 h of life. Another larger, retrospective analysis by the Canadian Neonatal Network (6) reported a U-shaped relationship betwixt body temperature (on admission to the NICU) and adverse event with the everyman agin outcome rates occurring at admission temperatures of 36.5–37.2°C. A more contempo study by the NICHD Neonatal research network (17) nevertheless plant a subtract of in-infirmary mortality with increasing admission temperatures even though the latter had risen in the past decade.
However, these studies refer to the atmospheric condition of primary care in the delivery room and/or admission to the NICU, respectively, and do not take into account the chronic exposure of preterm babies to potentially suboptimal thermal conditions during their long-lasting hospital stay. The usual textbook recommendations on thermal intendance on the NICU focus on "thermoneutrality" (14, fifteen). The thermoneutral temperature is defined as the ambient temperature that prevents any thermoregulatory (heat or cold) defense force reaction resulting in an increase in metabolic rate (eighteen). In view of the fact that the metabolic charge per unit cannot be routinely measured in preterm neonates, a stable body temperature (and, occasionally, a low core-to-shell temperature gradient) is commonly used equally a surrogate of thermoneutrality (19). However, the assumption that 37.0°C is the body core temperature that reflects thermoneutrality in preterm neonates irrespective of GA and BW (which might have been reasonable at a time when fifty-fifty this was hard to achieve), has never been endorsed past scientific data.
The consensus on target temperature in preterm infants, as found in our survey, deviates from the intrauterine temperature of the fetus which is causeless to exist 0.five–ane.0°C college than that of the female parent (which itself is slightly elevated during pregnancy) (ane–iii, 20). This would correspond to a fetal body temperature of at least 37.5°C. The WHO even describes 38.0°C every bit the prevalent fetal core temperature (four). In a contempo study by Topaloglu et al. (21) the mean rectal body temperature of newborn babies immediately after delivery was found to be 0.four–one.two°C higher than the mother's mean temperature, depending on the way of delivery. In the vaginal delivery group the babies had a mean rectal temperature of 37.five ± 0.6°C compared to the mean maternal temperature of 36.3 ± 0.three°C. As has been shown using telemetric methods in pregnant sheep, a core temperature slope betwixt the fetal and the maternal organism seems to be a characteristic of mammalian pregnancy (22, 23). The heat produced by the fetus has to exist removed either through the amniotic fluid and the uterine wall (conductive pathway) or via the umbilical arterial blood period to the placenta (convective pathway). As the heat electrical conductivity of the placenta is limited and its full resistance to heat menstruum is larger than zero, fetal temperature exceeds maternal temperature past about 0.five (0.3–ane.0)°C (2, 24).
Keeping these intrauterine conditions in mind, the homogeneity of target temperature values, as establish in our survey, is far from being self-evident. Under the designated target temperature range fifty-fifty infants built-in at 24 WOG who under normal circumstances would remain another 4 months in utero, are kept in the incubator at relevantly lower temperatures than physiologically prevalent at this stage of their evolution. Notably, the lower limit of our identified normal range (36.6°C) is more than than 1.0°C lower than the "convenance temperature" that the fetus would be exposed to in utero (37.5–38.0°C).
Upwardly to now, there are no animal and only a few clinical studies having tested college target values for torso temperature in preterm neonates. In a small observational written report with fourteen VLBWI, it was shown that when treated under conventional thermoneutral conditions, the infants' vasomotor tone, a surrogate for common cold stress, was high. When the infants' body temperatures were raised to 37.v–38.5°C the vasomotor tone was reduced and less problems were reported past the designated nursing staff (25). In a more recent study on 38 incubated preterm infants during their get-go 11 days of life, even a body temperature of 37.0°C was associated with considerably lower energy costs and greater weight proceeds, every bit compared with the 36.viii°C attained by a unlike incubator way (26).
The lack of scientific evidence contrasts to the considerable efforts to assess the optimal target values for other physiological parameters such as oxygen saturation (27) or carbon dioxide tension (28) that have been made in the by few years. Thus, thermal care appears to be a somewhat neglected neonatological practice that merits further study, not but with regard to short-term outcomes such equally weight gain and metabolic stress, but also to potential long-term consequences such equally neurological development.
On the other paw, our results prove that awareness for a higher thermal instability of the preterm infant does exist. The primary regulation of incubators was conducted choosing higher air temperature and relative humidity levels for more premature infants, a practice in line with conventional textbook recommendations (xiii–xv). Moreover, the cut-off point for hypothermia was defined at a slightly higher torso temperature value, the more young the infant is, although this difference did non accomplish statistical significance. Consistent with the findings of a French study from 2012 (16) a small inter-centre variability in the choice of air temperatures was nowadays, in the option of humidity values it was high. This variation underlines the lack of binding prove-based guidelines in the thermal management of pocket-size preterm infants. Although virtually centers refer to standard operating procedures (SOPs), 42% of them base their decisions regarding temperature targets and thermal management on the clinical assessment of the caretaker at bedside only.
Another remarkable finding of the written report is that the majority (68%) of participating NICUs prefer the ATC over the SSC mode of incubator operation, revealing the typical national practices in neonatal care. Moreover, only 16% of all centers report the use of central-peripheral gradient monitoring which has repeatedly been proposed not only as an appropriate indicator of thermal comfort (xiii, 25), but likewise as an early on predictor of late-onset sepsis in VLBWI (29, xxx).
Our survey seemed to be well-structured and comprehensive. This is reflected in the satisfactory quota of consummate responses even though the overall response rate (notably from Austrian NICUs) remained below our expectations. However, with a total of 87 eligible responses (out of 149 addressed perinatal centers, i.e., 58%) from Germany and Switzerland, it can exist considered equally representative for high-level perinatal centers in these countries.
The study has several other limitations: In VLBWI evaporative estrus loss is the predominant mode of rut loss during the first few days of life, which then decreases with increasing postnatal historic period. The high ambient temperatures and relative humidities initially needed to maintain an adequate body temperature in VLBWI can thus be gradually reduced over fourth dimension. As we asked for incubator settings on access simply, we did not capture the class of practical ambient temperatures and relative humidities with increasing postnatal age of the infants.
Inherent to the survey musical instrument, a potential social-desirability bias cannot be ruled out especially since the i responding was often not identical with the staff members responsible for thermal care at bedside. Moreover, as temperature ranges and cutting-off points for hypo- and hyperthermia were provided in preset temperature intervals and values, the participants could only select temperature or humidity values differing from another in 0.5°C or 5% intervals, respectively. As well the given premature subgroups may have confused participants, not knowing exactly where to identify a premature infant lying somewhere in between. The use of complimentary text boxes might have led to a larger variation of results.
Conclusion
In conclusion, as revealed by this survey, there is a tacit consensus amidst high-level NICUs that 37.0°C is the normal and thus desirable body temperature for VLBWI, irrespective of gestational historic period and/or birth weight. This is in dissimilarity to the fact that the intrauterine fetal torso temperature is assumed to be 0.5-1.0°C higher than the maternal ane and has not been assessed by prospective clinical studies relating target body temperature to short- and long-term outcomes.
Data Availability
The datasets generated for this study are available on request to the corresponding author.
Author Contributions
AP and FvdM contributed equally to the development of the questionnaire, assay of the data, and preparation of the manuscript. DS was involved in the planning of the report, discussion of the results, and finalization of the newspaper.
Funding
This inquiry did not receive any specific grant from funding agencies in the public, commercial, or non-turn a profit sectors.
Conflict of Interest Argument
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could exist construed as a potential disharmonize of interest.
Acknowledgments
The adept statistical support of East. Vettorrazzi (Institute of Medical Biometry and Epidemiology, University Medical Center Hamburg-Eppendorf) is gratefully acknowledged.
Supplementary Material
The Supplementary Material for this article can be plant online at: https://world wide web.frontiersin.org/articles/x.3389/fped.2019.00227/full#supplementary-material
References
4. World Wellness Organization (Maternal and Newborn Health / Safe Motherhood Unit). Thermal Protection of the Newborn: A Practical Guide. Geneva: WHO (1997). 68 p.
Google Scholar
5. Knobel RB, Holditch-Davis D, Schwartz TA. Optimal body temperature in transitional extremely low birth weight infants using eye rate and temperature equally indicators. J Obstet Gynecol Neonatal Nurs. (2010) 39:iii–14. doi: 10.1111/j.1552-6909.2009.01087.x
PubMed Abstruse | CrossRef Full Text | Google Scholar
6. Lyu Y, Shah PS, Ye XY, Warre R, Piedboeuf B, Deshpandey A, et al. (Canadian Neonatal Network). Association between admission temperature and mortality and major morbidity in preterm infants born at fewer than 33 weeks' gestation. JAMA Pediatr. (2015) 169:e150277. doi: ten.1001/jamapediatrics.2015.0277
CrossRef Total Text | Google Scholar
7. Silverman WA, Fertig JW, Berger AP. The influence of the thermal environment upon the survival of newly built-in premature infants. Pediatrics. (1958) 22:876–86.
PubMed Abstract | Google Scholar
8. Day RL, Caliguiri Fifty, Kamenski C, Ehrlich F. Body temperature and survival of premature infants. Pediatrics. (1964) 34:171–81.
PubMed Abstract | Google Scholar
9. Brück Yard. Temperature regulation in the newborn baby. Biol Neonat. (1961) iii:65–119.
Google Scholar
10. Hammarlund Thou, Stromberg B, Sedin G. Heat loss from the skin of preterm and fullterm newborn infants during the get-go weeks afterward birth. Biol Neonate. (1986) 50:1–10.
PubMed Abstract | Google Scholar
11. Branco de Almeida MF, Guinsburg R, Sancho GA, Rosa IRM, Lami ZC, Martinez Iron, et al. Hypothermia and early neonatal mortality in preterm infants. J Pediatr. (2014) 164:271–5.e1. doi: ten.1016/j.jpeds.2013.09.049
CrossRef Full Text | Google Scholar
12. Wilson E, Maier RF, Norman M, Misselwitz B, Howell EA, Zeitlin J, et al. Access hypothermia in very preterm infants and neonatal mortality and morbidity. J Pediatr. (2016) 175: 61–seven.e4. doi: 10.1016/j.jpeds.2016.04.016
PubMed Abstract | CrossRef Full Text | Google Scholar
13. A Okken and J Koch editors. Thermoregulation of Sick and Depression Nativity Weight Neonates. Berlin: Springer (1995). 241 p.
14. Gomella TL, Cunningham MD, Eyal FG. Neonatology: direction, procedures, on-call problems, diseases, and drugs, seventh ed. New York, NY: McGraw-Hill Education/Lange (2013). 1113 p.
15. Agren J. The thermal environment of the intensive intendance plant nursery. In: RJ Martin, AA Fanaroff, and MC Walsh editors. Fanaroff and Martin's Neonatal-Perinatal Medicine: Diseases of the Fetus and Infant, 10th ed. Philadelphia: Elsevier Saunders (2015). p. 502–12.
Google Scholar
sixteen. Deguines C, Décima P, Pelletier A, Dégrugilliers L, Ghyselen L, Tourneux P. Variations in incubator temperature and humidity direction: a survey of current exercise. Acta Paediatr. (2012) 101:230–5. doi: ten.1111/j.1651-2227.2011.02492.ten
PubMed Abstruse | CrossRef Full Text | Google Scholar
17. Laptook AR, Bell EF, Shankaran Due south, Boghossian NS, Wychoff MH, Kandefer S, et al. Admission temperature and associated mortality and morbidity among moderately and extremely preterm infants. J Pediatr. (2018) 192:53–nine.e2. doi: 10.1016/j.jpeds.2017.09.021
PubMed Abstract | CrossRef Full Text | Google Scholar
18. Gekle M, Singer D. Wärmehaushalt und Temperaturregulation. In: HC Pape, A Kurtz, and S Silbernagl editors. Physiologie. 8th ed. Stuttgart: Thieme (2018). p. 566–84.
19. Sauer PJ, Dane HJ, Visser HKA. New standards for neutral thermal surroundings of healthy very low birthweight infants in calendar week one of life. Curvation Dis Kid. (1984) 59:18–22.
PubMed Abstract | Google Scholar
20. Blackburn ST. Maternal, Fetal, & Neonatal Physiology: A Clinical Perspective. fifth ed. St. Louis: Elsevier Saunders (2018). 720 p.
Google Scholar
21. Topaloglu N, Binnetoglu FK, Yildirim Due south, Tekin M, Kaymaz N, Aylanç H, et al. Effect of delivery fashion on postpartum neonatal torso temperatures. J Matern Fetal Neonatal Med. (2016) 29:385–eight. doi: ten.3109/14767058.2014.1001359
PubMed Abstract | CrossRef Full Text | Google Scholar
22. Laburn HP, Mitchell D, Goelst K. Fetal and maternal body temperatures measured by radiotelemetry in virtually-term sheep during thermal stress. J Appl Physiol. (1992) 72:894–900.
PubMed Abstract | Google Scholar
23. Laburn HP, Faurie A, Goelst Thou, Mitchell D. Furnishings on fetal and maternal torso temperatures of exposure of pregnant ewes to heat, cold, and exercise. J Appl Physiol. (2002) 92:802–8. doi: x.1152/japplphysiol.00109.2001
PubMed Abstract | CrossRef Full Text | Google Scholar
24. Schröder HJ, Power GG. Engine and radiator: fetal and placental interactions for heat dissipation. Exp Physiol. (1997) 82:403–fourteen.
PubMed Abstruse | Google Scholar
25. Lemburg P. Thermal monitoring of very preterm infants: which temperature should be measured? In: A Okken and J Koch editors. Thermoregulation of Sick and Depression Nativity Weight Neonates. Berlin: Springer (1995). p. 63–eight.
Google Scholar
26. Degorre C, Décima P, Dégrugilliers L, Ghyselen L, Bach 5, Libert JP, et al. A mean body temperature of 37°C for incubated preterm infants is associated with lower energy costs in the first 11 days of life. Acta Paediatr. (2015) 104:581–8. doi: 10.1111/apa.12965
PubMed Abstract | CrossRef Full Text | Google Scholar
27. Askie LM, Darlow BA, Effectively N, Schmidt B, Stenson B, Tarnow-Mordi W, et al. Association betwixt oxygen saturation targeting and death or inability in extremely preterm infants in the neonatal oxygenation prospective meta-analysis collaboration. JAMA. (2018) 319:2190–201. doi: 10.1001/jama.2018.5725
PubMed Abstruse | CrossRef Full Text | Google Scholar
28. Thome UH, Genzel-Boroviczeny O, Bohnhorst B, Schmid M, Fuchs H, Rohde O, et al. Neurodevelopmental outcomes of extremely low birthweight infants randomised to dissimilar PCO2 targets: the PHELBI follow-upwardly study. Arch Dis Kid Fetal Neonatal Ed. (2017) 102:F376–82. doi: 10.1136/archdischild-2016-311581
PubMed Abstract | CrossRef Full Text | Google Scholar
29. Ussat Grand, Vogtmann C, Gebauer C, Pulzer F, Thome U, Knüpfer K. The role of elevated central-peripheral temperature difference in early detection of belatedly-onset sepsis in preterm infants. Early Hum Dev. (2015) 91:677–81. doi: x.1016/j.earlhumdev.2015.09.007
PubMed Abstract | CrossRef Full Text | Google Scholar
30. Leante-Castellanos JL, Martínez-Gimeno A, Cidrás-Pidré Yard, Martínez-Munar One thousand, García-González A, Fuentes-Gutiérrez C. Central-peripheral temperature monitoring as a marking for diagnosing late-onset neonatal sepsis. Pediatr Infect Dis J. (2017) 36:e293–7. doi: 10.1097/INF.0000000000001688
PubMed Abstract | CrossRef Total Text | Google Scholar
Source: https://www.frontiersin.org/articles/10.3389/fped.2019.00227/full
0 Response to "How Do Nicu Preemie Babies Regulate Their Body Temp"
Post a Comment